IUD = Intrauterine Device
Get to know the details on Mirena
The Mirena IUD is a type of long-acting reversible contraception. It’s over 99% effective at preventing pregnancy and can last for up to 8 years, plus it’s reversible—which means, if you want to stop using it, you can have Mirena removed at any time by your doctor. More about Mirena:
-
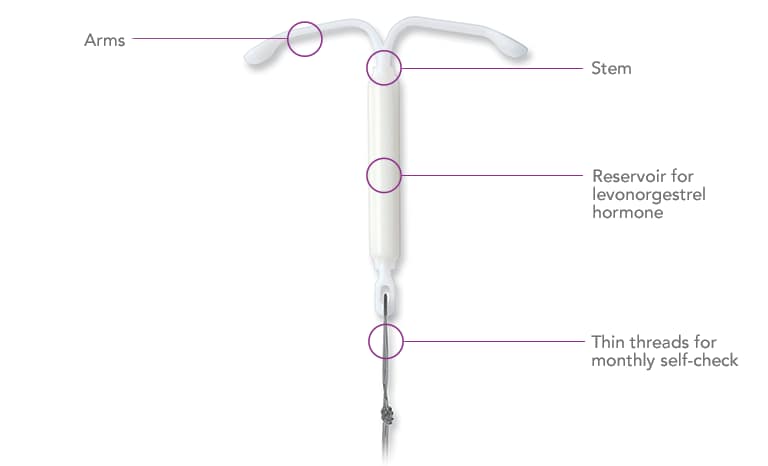
It is small, made of soft, flexible plastic, and T-shaped
-
It’s placed in your uterus by a doctor who can remove it at any time in case your plans change
-
Can be used whether or not you’ve had a baby
-
Can be placed during an in-office visit
You may experience pain, bleeding or dizziness during and after placement. If your symptoms do not pass within 30 minutes after placement, Mirena may not have been placed correctly. Your healthcare provider will examine you to see if Mirena needs to be removed or replaced.
Learn more about the Mirena placement process
How Small is Mirena?




A Mirena IUD is one of the most effective forms of birth control
-
Is over 99% effective at preventing pregnancy for up to 8 years
-
Less than 1 pregnancy per 100 women in a year
-
FDA-approved to treat heavy periods—also known as heavy menstrual bleeding (HMB)—for up to 5 years in women who choose an IUD for birth control
Some serious risk considerations about Mirena
Although pregnancy while using Mirena is uncommon (less than 1 in 100), it can be serious. Call your healthcare provider right away if you think you may be pregnant. If possible, also do a urine pregnancy test.
If you get pregnant while using Mirena, you may have an ectopic pregnancy. This means that the pregnancy is not in the uterus. Unusual vaginal bleeding or abdominal pain, especially with missed periods, may be a sign of ectopic pregnancy. Ectopic pregnancy is a medical emergency that often requires surgery. Ectopic pregnancy can cause internal bleeding, infertility, and even death.
There are also risks if you get pregnant while using Mirena and the pregnancy is in the uterus. Severe infection, miscarriage, premature delivery, and even death can occur with pregnancies that continue with an intrauterine device (IUD). Because of this, your healthcare provider may try to remove Mirena, even though removing it may cause a miscarriage. If Mirena cannot be removed, talk with your healthcare provider about the benefits and risks of continuing the pregnancy and possible effects of the hormone on your unborn baby. If you continue your pregnancy, see your healthcare provider regularly.
Call your healthcare provider right away if you get flu-like symptoms, fever, chills, cramping, pain, bleeding, vaginal discharge, or fluid leaking from your vagina. These may be signs of infection.
See the full list of serious risk considerations for Mirena.
Mirena is a pill-free birth control option
In a study of over 4,500 women around the world, including 500 women in the United States aged 21–29 years who take a daily birth control pill, 82% of US women reported* forgetting to take it at least once in the past 12 months.†
Mirena lasts up to 8 years for pregnancy prevention, and eliminates the responsibility of taking a daily pill—that’s 2,920 daily pills over 8 years vs 1 Mirena IUD. You will need to do a thread check 1 time a month to make sure Mirena is still in place. Your healthcare provider can tell you how.
Within 4 to 6 weeks of placement, you should return for a follow-up visit. If you don't feel the threads or feel more than just the threads, call your healthcare provider. Mirena may not be in the right position and may not prevent pregnancy. Avoid intercourse or use non-hormonal back-up birth control (such as condoms or spermicide) until your healthcare provider can check that Mirena is still in the right place.
*When asked, "In the past 12 months, have you ever forgotten to take your pill?"
†Based on a study conducted by Opinion Health on behalf of Bayer Pharmaceuticals Division, conducted in June/July 2016.
INDICATIONS FOR MIRENA
Mirena® (levonorgestrel-releasing intrauterine system) is a hormone-releasing IUD that prevents pregnancy for up to 8 years. Mirena also treats heavy periods for up to 5 years in women who choose intrauterine contraception.
IMPORTANT SAFETY INFORMATION
- If you have a pelvic or genital infection, get infections easily, or have certain cancers, don't use Mirena. Less than 1% of users get a serious pelvic infection called pelvic inflammatory disease (PID).
- If you have persistent pelvic or stomach pain, or excessive bleeding after placement, tell your healthcare provider (HCP). If Mirena comes out, call your HCP and avoid intercourse or use non-hormonal back-up birth control (such as condoms or spermicide). Mirena may go into or through the wall of the uterus and cause other problems.
-
Pregnancy while using Mirena is uncommon but can be life threatening and may result in loss of pregnancy or fertility.
- Ovarian cysts may occur but usually disappear.
- Bleeding and spotting may increase in the first 3 to 6 months and remain irregular. Periods over time usually become shorter, lighter, or may stop.
Mirena does not protect against HIV or STIs.
Only you and your HCP can decide if Mirena is right for you. Mirena is available by prescription only.
For important risk and use information about Mirena, please see Full Prescribing Information.







