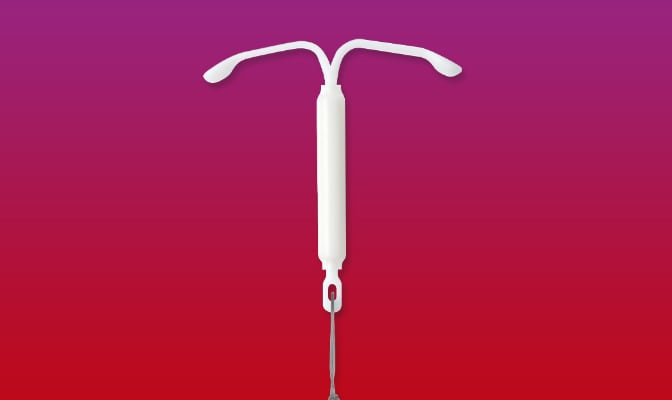
Over 99% effective at preventing pregnancy for up to 8 years.
FDA-approved to decrease menstrual blood loss for up to 5 years in women who have heavy periods and choose an IUD for birth control.
†Supported by 2020-2022 SHS data.
Mirena is not right for everyone. Do not use Mirena if you:
are or might be pregnant; Mirena cannot be used as an emergency contraceptive
have a serious pelvic infection called pelvic inflammatory disease (PID) or have had PID in the past unless you have had a normal pregnancy after the infection went away
have an untreated genital infection now
have had a serious pelvic infection in the past 3 months after a pregnancy
can get infections easily. For example, if you:
have multiple sexual partners or your partner has multiple sexual partners
have problems with your immune system
use or abuse intravenous drugs
have or suspect you might have cancer of the uterus or cervix
have bleeding from the vagina that has not been explained
have liver disease or a liver tumor
have breast cancer or any other cancer that is sensitive to progestin (a female hormone), now or in the past
have an intrauterine device in your uterus already
have a condition of the uterus that changes the shape of the uterine cavity, such as large fibroid tumors
are allergic to levonorgestrel, silicone, polyethylene, silica, barium sulfate or iron oxide
Keeping it real: what actual users are saying about Mirena
Listen to what these women have to say as they tell their story and share their real experiences with Mirena.
The women shown below use or have used Mirena and have been compensated for their time. Individual experience may vary.

“I talk to my patients who have heavy periods and want an IUD for their birth control about Mirena. If you have questions about heavy menstrual bleeding or the Mirena IUD, talk to your doctor…” - Dr. Nicole Alicia (@nicolealiciamd), MD, a Board Certified OBGYN

“Everyone’s experience is different, but for me Mirena is the right birth control choice as a busy mom.” - Influencer and Midwife Caitlyn (@themodernmidwife) on using Mirena as her birth control

“Two years ago I got the Mirena IUD. It’s been one of the best choices I’ve made for myself since talking with my doctor.” - Influencer Violet (@violetsummersby) on using Mirena for birth control and for heavy menstrual bleeding treatment
How much does Mirena cost?
Find out if your insurance covers the cost of Mirena, and what to do if you don’t have coverage.
INDICATIONS FOR MIRENA
Mirena® (levonorgestrel-releasing intrauterine system) is a hormone-releasing IUD that prevents pregnancy for up to 8 years. Mirena also treats heavy periods for up to 5 years in women who choose intrauterine contraception.
IMPORTANT SAFETY INFORMATION
- If you have a pelvic or genital infection, get infections easily, or have certain cancers, don't use Mirena. Less than 1% of users get a serious pelvic infection called pelvic inflammatory disease (PID).
- If you have persistent pelvic or stomach pain, or excessive bleeding after placement, tell your healthcare provider (HCP). If Mirena comes out, call your HCP and avoid intercourse or use non-hormonal back-up birth control (such as condoms or spermicide). Mirena may go into or through the wall of the uterus and cause other problems.
-
Pregnancy while using Mirena is uncommon but can be life threatening and may result in loss of pregnancy or fertility.
- Ovarian cysts may occur but usually disappear.
- Bleeding and spotting may increase in the first 3 to 6 months and remain irregular. Periods over time usually become shorter, lighter, or may stop.
Mirena does not protect against HIV or STIs.
Only you and your HCP can decide if Mirena is right for you. Mirena is available by prescription only.
For important risk and use information about Mirena, please see Full Prescribing Information.